Hip and knee arthroplasties – i.e., artificial joint replacements, as they are used in therapy for osteoarthritis – have been performed for decades and represent proven procedures. Nevertheless, the demanding conditions under which hip and knee arthroplasties are used repeatedly lead to complications that can cause the implants to fail. These include stress shielding – a loss of bone density in the immediate vicinity of the implant – and bacterial infections of the surrounding tissue.
In these cases, the load-bearing capacity of the implants is often significantly reduced. This can cause patients to experience high levels of pain. As a result, prostheses often have to be removed to prepare for the insertion of a replacement prosthesis.
Mechanical implant revision can damage surrounding tissue
These revision surgeries account for roughly10 percent of the total hip and knee replacement surgeries performed in Germany each year. Nevertheless, revision surgeries still play a minor role in the development of prostheses, and explantations are usually performed purely mechanically. In this procedure, the surgeon pulls the partially exposed implant out of its seat using mechanical force, such as a draw hammer, and also uses chisels and burs to chip and grind away the surrounding bone cement.
This procedure carries a considerable risk of damaging the surrounding bone by erosion or fracture. Increased bone loss is associated with larger revision prostheses and more costly surgeries as well as longer reconvalescence times. The goal is therefore to preserve as much healthy bone tissue as possible.
Research goal: gentler procedure for removing implants
The aim of project A08 in the collaborative research center SIIRI (Safety-Integrated and Infection-Reactive Implants) is to develop a gentler explantation procedure using inductive heating processes. To this end, the IW is transferring its experience in the field of inductive heat treatment of metals to hip and knee endoprostheses. IW researchers are supported by the biomechanical and medical expertise of researchers from the Laboratory of Biomechanics and Biomaterials (LBB) at Hannover Medical School.
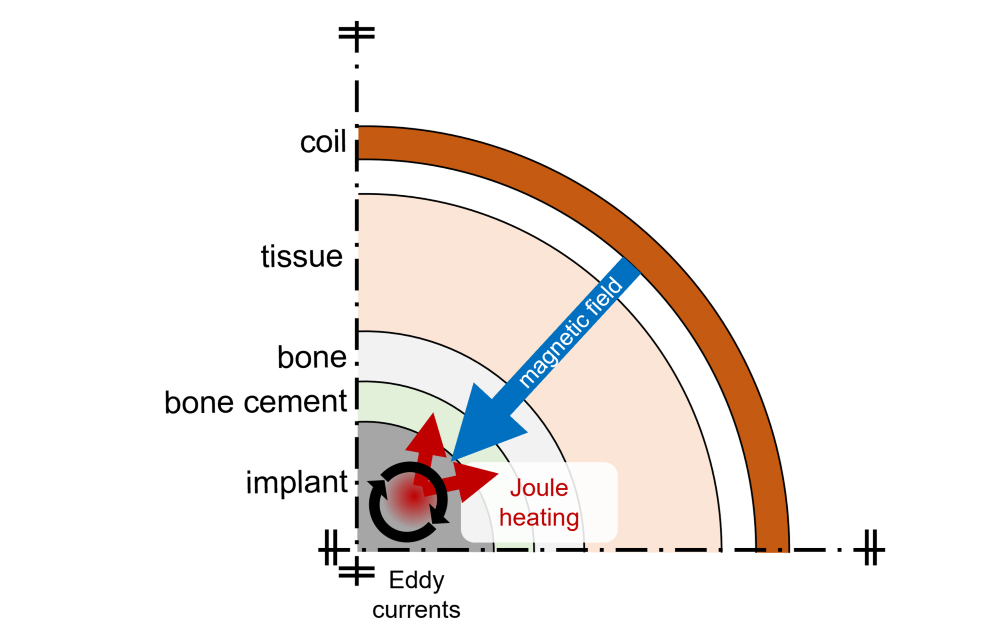
Induction heating involves passing a high-frequency alternating current through a coil. This creates eddy currents that heat metallic materials without contact. Induction stoves work according to this principle as well. In the same way, eddy currents can be generated in the implant surface that heat metallic implants withoutdirectly interacting with the surrounding tissue.
Implants detach more easily after targeted induction heating
The implant conducts the generated heat into the bone cement and softens it, which in turn makes it easier to loosen the bond between implant, bone cement and bone. In preliminary tests on cylinders made of Ti-6Al-4V, a titanium alloy frequently used in implant technology, IW researchers have achieved a reduction in the necessary pull-out force of about 50 percent. This would almost completely eliminate the need to chisel out the bone cement in revision operations.
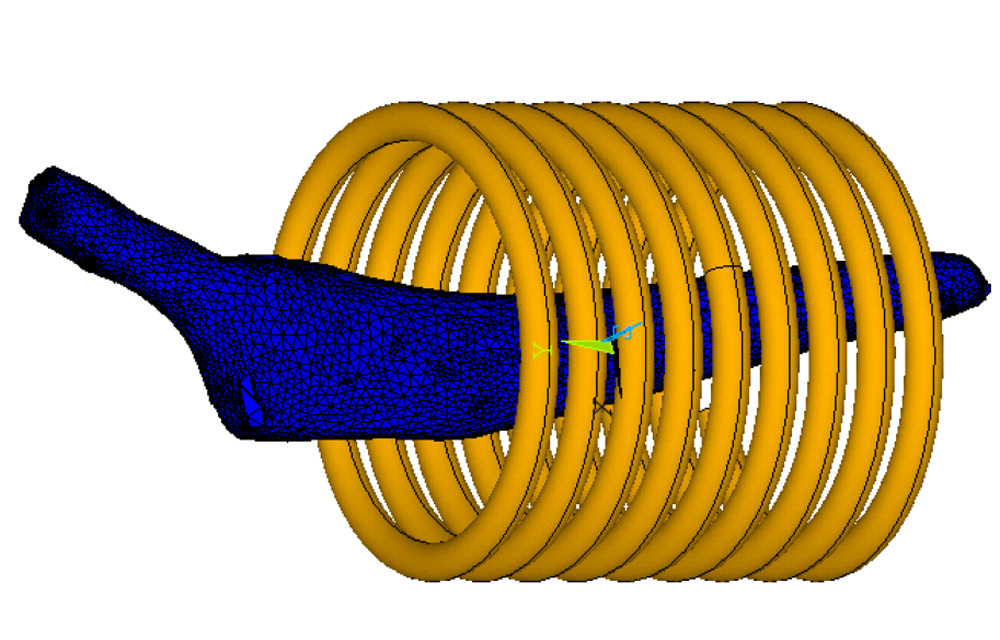
However, since the thermal energy introduced can also cause damage to the surrounding bone, muscle and nerve tissue, it is essential that the heat output is precisely controlled. To ensure this, the IW is developing simulations that can be used to predict the temperature distributions achieved in the implant and bone cement. This simulation model enables a definition of the heating parameters and a design of the required coils for different implant types and installation situations.
In addition to the development of the simulation, IW and LBB are performing validation in several surrogate models. Various heating and pull-out tests are planned for this purpose, the results of which will be used to improve the simulations.
Perspective: Avoid bone damage, accelerate recovery
In the future, simulation should make it possible to predict an adapted heating strategy for endoprostheses in the perioperative environment of revisions. By tailoring the use of this technology to individual patients, it will be possible to avoid bone damage during revision surgery and thus significantly shorten recovery periods in the future.